FIRES
Fever induced refractory epileptic encephalopathy in school age children
Fever induced refractory epileptic encephalopathy in school age children (FIRES) is a devastating condition which follows a prolonged refractory status epilepticus (SE) triggered by fever of unknown cause. The intractable perisylvian status epilepticus might persist for more than a month and results in severe cognitive impairment.
History
Several authors[1][2][3][4][5][4] have reported a presumed post encephalitic catastrophic epileptic encephalopathy resulting in refractory repetitive seizures associated with severe cognitive impairment.
Mikaeloff et al[3] in 2006 described this condition in a retrospective study of normally developing 14 children (mean age 7.5yrs) admitted with prolonged status epilepticus following a nonspecific febrile illness and called it Devastating Epileptic encephalopathy in School-age Children (DESC).
The current term febrile infection-related epilepsy syndrome (FIRES) was proposed by Van Baalen et al[6] in 2010 who published a retrospective multicenter case series of 22 previously healthy children aged 3-15yrs (largest of the series) who developed prolonged and recurrent refractory seizures occurring 2-14 days (median 5 days) after fever onset.
Pathophysiology
Absence of either encephalitic changes in neuroimaging,marked CSF leukocytosis or inflammatory changes on biopsy suggests that the pathological process is not one of inflammation. The clinical course is characterised by intractable recurrent/prolonged seizures suggesting neuronal hyperexcitation as the underlying cause.It is possible that the pathogenesis is immune mediated.
Clinical characteristics
- The condition occurs in previously healthy normally developing children aged 3-15 years.
- Characterised by an acute convulsive status epilepticus following a short febrile episode without any evidence of cns infection or inflammation.
- The status epilepticus is highly pharmacoresistant and can persist for more than a month
- The seizures are characteristically bilateral perisylvian with propagation to the frontal lobes and are extremely frequent and refractory
- The acute phase is followed by a chronic pharmacoresistant epilepsy associated with severe cognitive impairment mainly involving language, memory and behaviour.
- There is no latent period between the progression from acute to chronic phase.
Neurophysiology
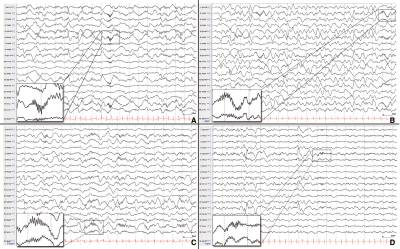
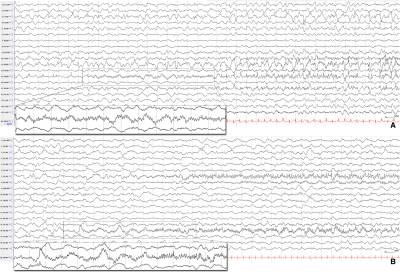
- EEG shows diffuse slowing or multifocal discharges
- Extreme delta brush (EDB) in the background is frequently seen in the acute presentation[7]
- prolonged focal fast activity and hemispheric shifting ictal activity is characteristic and is a potential early biomarker in patients with FIRES[7]

Neuroimaging
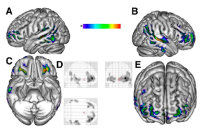
Plain MRI is often normal, although selective bilateral hippocampal abnormalities including atrophy and hypersignal have been reported.18F-FDG PET studies[8] have shown widepsread interictal hypometabolic network including the temporoparietal and orbitofrontal cortices bilaterally. The hypometabolic areas corresponded to the electroclinical seizures involving the temporofrontal cortex bilaterally as well as to the neuropsychologic findings.
Neuropsychology
Neuropsychological deficits mainly involve language, frontal functions, behaviour and memory
FIRES and NORSE
An consensus definition of FIRES proposed by a group of experts in 2018[9] excludes most cases of febrile status epilepticus in children (prolonged febrile convulsions), as febrile seizures usually occur in children who have onset of fever <24 hours prior to onset of seizures or whose fever is recognized only after the onset of seizures. New‐onset refractory status epilepticus(NORSE) is a clinical presentation, not a specific diagnosis, in a patient without active epilepsy or other preexisting relevant neurological disorder, with new onset of refractory status epilepticus without a clear acute or active structural, toxic, or metabolic cause.
Treatment
- FIRES is characteristically highly refractory to treatment.
- The efficacy of ketogenic diet as an alternative to pharmacotherapy in FIRES has been reported with favourable outcomes[10][11]. There are no randomized controlled trials available on the use of the ketogenic diet in status epilepticus[reference needed].
- Deep brain stimulation of the centromedian thalamic nuclei (CMN-DBS) has been reported in some cases with where generalised seizures have been abolished but did not have a lasting effect on focal seizures burden[12]
- Gofshteyn et al.(2017) reported an open label case series where cannabadiol (Epidiolex, GW Pharma) was used alongside other anti-seizure medications on emergency or expanded investigational protocols in either the acute or chronic phase of illness and showed improvement in seizure frequency and duration[13]
References
|
1.
a
. AERRPS, DESC, NORSE, FIRES: multi-labeling or distinct epileptic entities?. Epilepsia. 2011 Nov;52(11):e185-9. doi: 10.1111/j.1528-1167.2011.03293.x. Epub 2011 Oct 17.
[PMID: 22004046] [DOI: 10.1111/j.1528-1167.2011.03293.x]
2.
a
. The acute encephalopathies of obscure origin in infants and children. Brain. 1961 Dec;84:680-708. doi: 10.1093/brain/84.4.680.
[PMID: 14467623] [DOI: 10.1093/brain/84.4.680]
3.
a,
b
. Devastating epileptic encephalopathy in school-aged children (DESC): a pseudo encephalitis. Epilepsy Res. 2006 Apr;69(1):67-79. doi: 10.1016/j.eplepsyres.2006.01.002. Epub 2006 Feb 15.
[PMID: 16469483] [DOI: 10.1016/j.eplepsyres.2006.01.002]
4.
a,
b
. Severe refractory status epilepticus owing to presumed encephalitis. J Child Neurol. 2005 Mar;20(3):184-7. doi: 10.1177/08830738050200030301.
[PMID: 15832606] [DOI: 10.1177/08830738050200030301]
5.
a
. Acute encephalitis with refractory, repetitive partial seizures: case reports of this unusual post-encephalitic epilepsy. Brain Dev. 2007 Apr;29(3):147-56. doi: 10.1016/j.braindev.2006.08.005. Epub 2006 Sep 27.
[PMID: 17008042] [DOI: 10.1016/j.braindev.2006.08.005]
6.
a
. Febrile infection-related epilepsy syndrome (FIRES): a nonencephalitic encephalopathy in childhood. Epilepsia. 2010 Jul;51(7):1323-8. doi: 10.1111/j.1528-1167.2010.02535.x. Epub 2010 Mar 18.
[PMID: 20345937] [DOI: 10.1111/j.1528-1167.2010.02535.x]
7.
a,
b
. Early ictal and interictal patterns in FIRES: The sparks before the blaze. Epilepsia. 2017 Aug;58(8):1340-1348. doi: 10.1111/epi.13801. Epub 2017 May 26.
[PMID: 28555777] [DOI: 10.1111/epi.13801] |
8.
a
. 18F-FDG PET reveals frontotemporal dysfunction in children with fever-induced refractory epileptic encephalopathy. J Nucl Med. 2011 Jan;52(1):40-7. doi: 10.2967/jnumed.110.077214. Epub 2010 Dec 13.
[PMID: 21149491] [DOI: 10.2967/jnumed.110.077214]
9.
a
. Proposed consensus definitions for new-onset refractory status epilepticus (NORSE), febrile infection-related epilepsy syndrome (FIRES), and related conditions. Epilepsia. 2018 Apr;59(4):739-744. doi: 10.1111/epi.14016. Epub 2018 Feb 5.
[PMID: 29399791] [DOI: 10.1111/epi.14016]
10.
a
. Efficacy of ketogenic diet in severe refractory status epilepticus initiating fever induced refractory epileptic encephalopathy in school age children (FIRES). Epilepsia. 2010 Oct;51(10):2033-7. doi: 10.1111/j.1528-1167.2010.02703.x. Epub 2010 Aug 31.
[PMID: 20813015] [DOI: 10.1111/j.1528-1167.2010.02703.x]
11.
a
. The ketogenic diet improves recently worsened focal epilepsy. Dev Med Child Neurol. 2009 Apr;51(4):276-81. doi: 10.1111/j.1469-8749.2008.03216.x. Epub 2008 Feb 3.
[PMID: 19191829] [DOI: 10.1111/j.1469-8749.2008.03216.x]
12.
a,
b
. Centromedian thalamic nuclei deep brain stimulation and Anakinra treatment for FIRES - Two different outcomes. Eur J Paediatr Neurol. 2019 Sep;23(5):749-754. doi: 10.1016/j.ejpn.2019.08.001. Epub 2019 Aug 8.
[PMID: 31446001] [DOI: 10.1016/j.ejpn.2019.08.001]
13.
a
. Cannabidiol as a Potential Treatment for Febrile Infection-Related Epilepsy Syndrome (FIRES) in the Acute and Chronic Phases. J Child Neurol. 2017 Jan;32(1):35-40. doi: 10.1177/0883073816669450. Epub 2016 Sep 29.
[PMID: 27655472] [DOI: 10.1177/0883073816669450] |

Discussion